Your basket is currently empty!
Cardiovascular Disease
Atherosclerosis
The prefix athero- means soft or “porridge-like,” while -sclerosis refers to hardening. Atherosclerosis describes the combination of atheromas (fatty accumulations within arterial walls) and sclerosis (thickening and loss of elasticity of the vessel wall).
Atherosclerosis mainly involves medium and large arteries. It develops due to long-term inflammation and immune system activation within the arterial wall. This drives lipid deposition in the vessel lining and subsequent formation of fibrous atheromatous plaques.
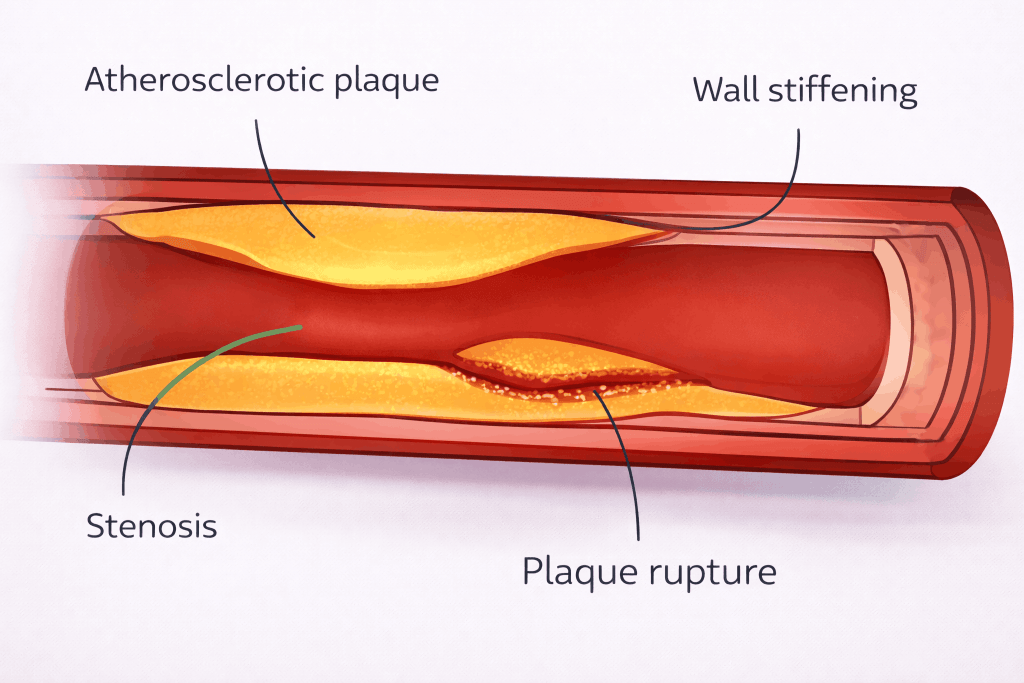
These plaques lead to:
- Stiffening
- Stenosis
- Plaque rupture
Stiffening reduces arterial compliance, contributing to hypertension (raised blood pressure) and increasing the workload on the heart, which must pump against higher resistance.
Stenosis narrows the arterial lumen and therefore reduces blood flow, for example causing angina.
When a plaque ruptures, a thrombus can form and obstruct a downstream vessel, resulting in ischaemia. A key example is acute coronary syndrome, where a coronary artery becomes occluded.
Risk Factors
Risk factors for cardiovascular disease are best divided into non-modifiable and modifiable factors. Non-modifiable risks cannot be changed, whereas modifiable risks can be targeted to reduce overall risk.
Non-modifiable risk factors
- Increasing age
- Family history
- Male sex
Modifiable risk factors
- High cholesterol
- Smoking
- Alcohol intake
- Unhealthy diet
- Physical inactivity
- Obesity
- Poor sleep
- Stress
Medical Co-Morbidities
Certain medical conditions raise the risk of developing atherosclerosis and should be optimally managed to reduce that risk:
- Diabetes
- Hypertension
- Chronic kidney disease (CKD)
- Inflammatory diseases (e.g., rheumatoid arthritis)
- Atypical antipsychotic medication use
TOP TIP: When taking a history from someone with suspected atherosclerotic disease (for example, a patient with chest pain), actively explore cardiovascular risk factors. Ask about exercise, diet, past medical history, family history, occupation, smoking status, alcohol use, and current medications. This approach is helpful both in exams and when presenting cases to senior clinicians.
Outcomes of Atherosclerosis
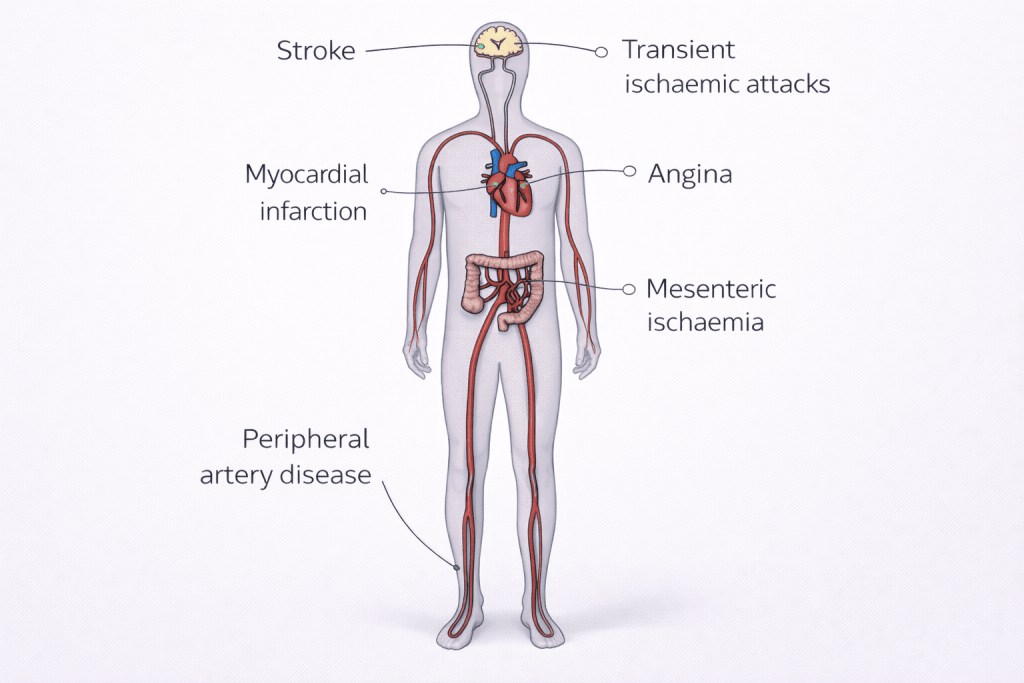
Atherosclerosis can ultimately result in:
- Angina
- Myocardial infarction
- Transient ischaemic attacks (TIAs)
- Stroke
- Peripheral arterial disease
- Chronic mesenteric ischaemia
Prevention of Cardiovascular Disease
Cardiovascular prevention is usually grouped into two categories:
- Primary prevention: for individuals who have never been diagnosed with cardiovascular disease
- Secondary prevention: after diagnoses such as angina, myocardial infarction, TIA, stroke, or peripheral arterial disease
Optimising Modifiable Risk Factors
Whether aiming for primary or secondary prevention, it is essential to address modifiable risk factors:
- Improve diet, increase exercise, and manage obesity
- Stop smoking
- Reduce alcohol intake
- Optimise treatment of co-morbidities (e.g., diabetes)
Diet and Exercise
NICE cardiovascular disease guidance (updated February 2023) advises the following dietary measures:
- Total fat intake under 30% of total calories, mainly from monounsaturated and polyunsaturated fats
- Saturated fat intake under 7% of total calories
- Lower sugar consumption
- Choose wholegrain foods
- At least 5 portions of fruit and vegetables daily
- At least 2 servings of fish per week, including one oily fish
- At least 4 servings per week of legumes, seeds, and nuts
NICE also recommends (as tolerated and limited by co-morbidities):
- Aerobic activity totalling at least 150 minutes/week at moderate intensity, or 75 minutes/week at vigorous intensity
- Strength/resistance training on at least 2 days per week
Primary Prevention of Cardiovascular Disease
Drug therapy for primary prevention is guided by the QRISK3 score.
The QRISK score estimates a patient’s 10-year percentage risk of having a stroke or myocardial infarction. NICE guidance (February 2023) recommends that if QRISK is above 10%, patients should be offered a statin—starting with atorvastatin 20 mg at night.
Atorvastatin 20 mg is offered as primary prevention to all patients with:
- Chronic kidney disease (eGFR < 60 ml/min/1.73 m²)
- Type 1 diabetes for more than 10 years or age over 40 years
Draft NICE guidance due for publication in mid-2023 suggests considering atorvastatin 20 mg for primary prevention even when QRISK3 is below 10%.
Statins
Statins lower cholesterol by inhibiting HMG-CoA reductase, reducing hepatic cholesterol synthesis.
NICE recommends repeating lipid testing 3 months after starting a statin and increasing the dose to achieve a >40% reduction in non-HDL cholesterol. Before up-titrating, confirm adherence (i.e., that the patient is actually taking the medication).
NICE also advises checking LFTs within 3 months of initiation and again at 12 months. Statins can cause a mild, temporary rise in ALT/AST during the first few weeks. They usually do not need stopping unless the rise is more than 3 times the upper limit of normal.
Rare but important adverse effects include:
- Myopathy (muscle pain and weakness)
- Rhabdomyolysis (muscle breakdown—check creatine kinase if muscle symptoms occur)
- Type 2 diabetes
- Haemorrhagic stroke (very rare)
In most cases, the benefits of statins significantly outweigh their risks, and modern statins such as atorvastatin are typically well tolerated.
TOP TIP: Statins interact with several commonly used medicines. A particularly important interaction is with macrolide antibiotics. If a patient is prescribed clarithromycin or erythromycin, they should be advised to pause their statin while taking the antibiotic course.
Other Cholesterol-Lowering Medications
- Ezetimibe reduces cholesterol absorption in the gut. It can be used instead of statins if statins are not tolerated, or alongside a statin if statins alone do not achieve adequate lipid lowering.
- Ezetimibe can be combined with bempedoic acid, which decreases cholesterol production in the liver.
- PCSK9 inhibitors (e.g., evolocumab and alirocumab) are monoclonal antibodies that markedly reduce cholesterol levels. They are specialist treatments administered by subcutaneous injection every 2–4 weeks.
Secondary Prevention of Cardiovascular Disease
Secondary prevention depends on the specific cardiovascular diagnosis. A useful way to remember core components is the “4 As”:
- A – Antiplatelet therapy (e.g., aspirin, clopidogrel, ticagrelor)
- A – Atorvastatin 80 mg
- A – Atenolol (or another beta blocker—commonly bisoprolol) titrated to the maximum tolerated dose
- A – ACE inhibitor (commonly ramipril) titrated to the maximum tolerated dose
After a myocardial infarction, dual antiplatelet therapy is initially used:
- Aspirin 75 mg daily (continued indefinitely)
- Clopidogrel or ticagrelor, usually for 12 months before stopping
Clopidogrel is the preferred antiplatelet agent in peripheral arterial disease and after an ischaemic stroke.
Familial Hypercholesterolaemia
Familial hypercholesterolaemia is an autosomal dominant inherited disorder that causes markedly raised cholesterol. Multiple different genes can be responsible.
- Heterozygous FH means one abnormal gene copy; it affects roughly 1 in 250 people.
- Homozygous FH means both copies are abnormal; it is very rare and causes extremely high cholesterol (often >13 mmol/L) with an almost inevitable risk of early cardiovascular disease.
Clinical diagnosis is made using the Simon Broome criteria or the Dutch Lipid Clinic Network criteria. Three key features to remember are:
- Family history of premature cardiovascular disease (e.g., MI before age 60 in a first-degree relative)
- Very high cholesterol (e.g., >7.5 mmol/L in an adult)
- Tendon xanthomata—firm cholesterol deposits within tendons, often on the Achilles tendon or the back of the hand
Management includes:
- Specialist referral for genetic testing and screening of relatives
- Statin therapy
Last updated Dec 2025
